The recommendation for infants born to women who test positive for hepatitis B surface antigen—or whose status is unknown—remains unchanged. Those newborns are still expected to receive both hepatitis B immune globulin and the first vaccine dose within 12 hours of delivery. The panel reiterated that prompt immunization in this group is critical to prevent mother-to-child transmission, which can lead to chronic infection and serious liver disease later in life.
Risk factors outlined
ACIP documents circulated at the meeting include a footnote advising parents and clinicians to consider additional household and community risks when deciding about the birth dose for babies of hepatitis B-negative mothers. Factors listed are:
- A household member known to be hepatitis B positive.
- Close, frequent contact with individuals who migrated from regions where hepatitis B is highly prevalent.
Second vote on antibody testing
In a separate action, the committee voted 6–4, with one abstention, to recommend that parents of older children who did not receive the birth dose discuss hepatitis B antibody testing with their pediatrician before initiating or completing the vaccination series. The proposed testing would verify whether the child has already mounted adequate antibody levels—either through vaccination or unrecognized infection—potentially reducing unnecessary additional doses. ACIP specified that insurers should cover the cost of this laboratory assessment.
Next steps
The updated recommendations are not final until they are reviewed and signed by CDC Acting Director and Health and Human Services Deputy Secretary Jim O’Neill. Once approved, the guidance will be published in the CDC’s Morbidity and Mortality Weekly Report and incorporated into the national childhood immunization schedule.
Background on hepatitis B vaccination
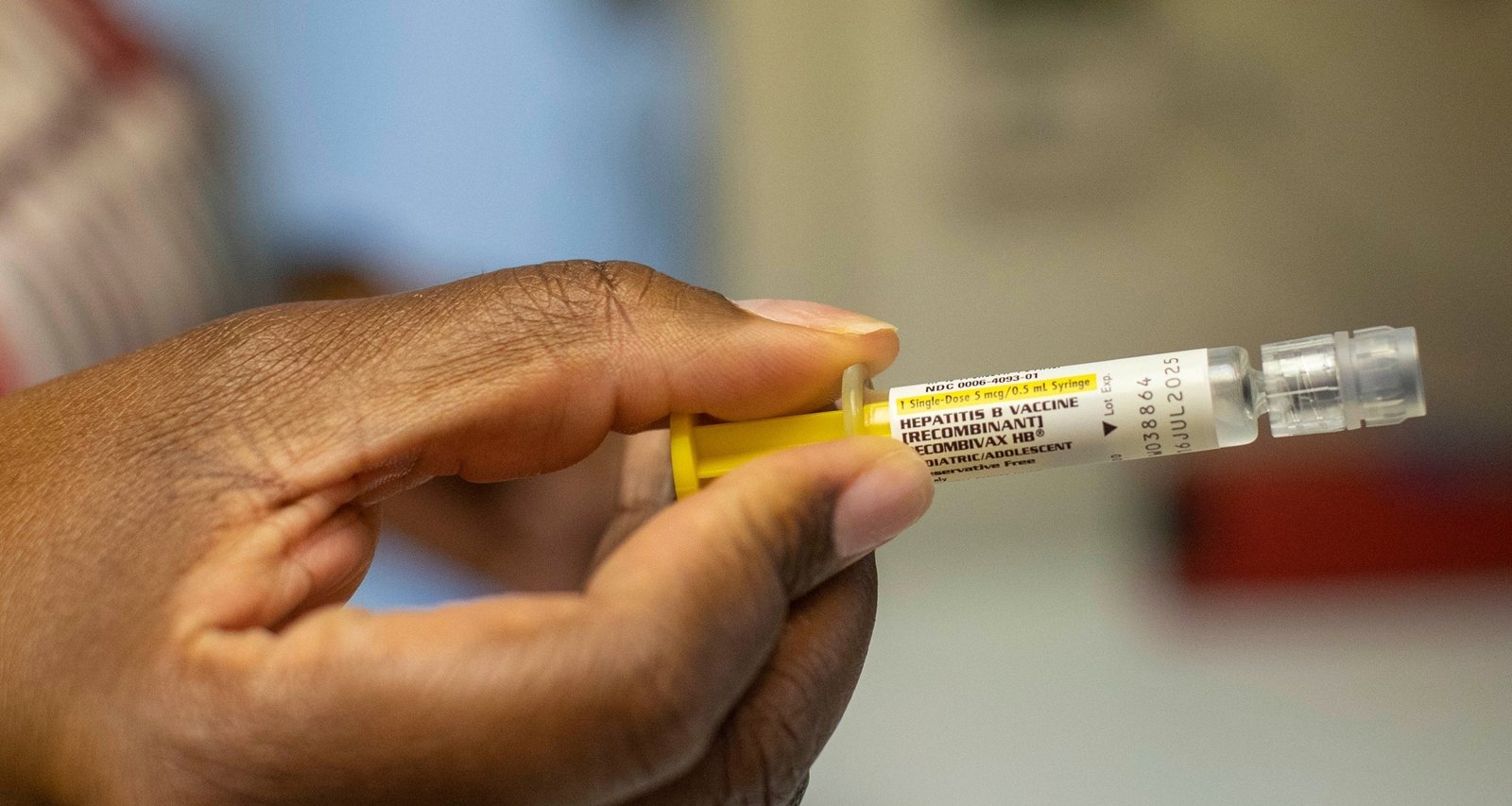
Imagem: Internet
Hepatitis B is a viral infection that can cause both acute and chronic liver disease. The birth dose, introduced in the United States in 1991, has been credited with reducing perinatal transmission and childhood infection rates. According to the CDC, chronic hepatitis B affects an estimated 862,000 people nationwide, many of whom were infected at birth or in early childhood. More information on the disease and its prevention is available from the CDC’s hepatitis division (CDC Hepatitis Resources).
Before the vote, ACIP members reviewed epidemiologic data indicating that nearly all perinatal hepatitis B infections occur among infants born to mothers who are surface antigen positive or whose infection status was not identified before delivery. Proponents of the change argued that universal vaccination at birth offers limited additional benefit when maternal screening is widespread and accurate. Opponents expressed concern that relying on prenatal test results could create gaps in protection if documentation is incomplete or if errors occur during labor and delivery.
Implementation considerations
Hospitals and birthing centers will need to adjust standing orders that currently call for automatic administration of the birth dose. Clinicians must confirm maternal hepatitis B test reports and engage parents in timely discussions about vaccination. The committee underscored that facilities should maintain protocols to ensure rapid immunization for infants at risk because of positive or unknown maternal status.
Public health agencies are expected to develop educational materials for obstetric and pediatric providers to support consistent application of the new guidance. Monitoring systems, including state immunization registries, may require updates to track deferred birth doses and follow-up vaccinations at later well-child visits.
Insurance coverage and access
While ACIP recommendations generally drive private insurance and public program coverage, formal adoption by the CDC director is required before payers are obligated to reimburse services. The committee’s inclusion of antibody testing as a recommended, insurer-covered service aims to minimize financial barriers for families who consider that option.
ACIP convenes three times a year to evaluate evidence on vaccine safety, efficacy and public health impact. Its 15 voting members include pediatricians, internists, family physicians, epidemiologists and public health experts appointed by the U.S. Department of Health and Human Services.
Crédito da imagem: Alyssa Pointer for The Washington Post via Getty Images



